Systemic Inflammatory Response Syndrome (SIRS)
- Rajyalakshmi Mannem
- Jan 13
- 8 min read
Systemic Inflammatory Response Syndrome (SIRS) is a clinical condition characterized by widespread inflammation throughout the body. It is identified by abnormal vital signs and laboratory markers such as temperature, heart rate, respiratory rate, and white blood cell count. Early recognition of SIRS is crucial, as it can signal serious underlying conditions like infection or sepsis, and prompt timely intervention to improve patient outcomes.
What is SIRS?
SIRS (systemic inflammatory response syndrome) is an exaggerated defense response from your body to a harmful stressor. It causes severe inflammation throughout your body. This can lead to reversible or irreversible organ failure and even death.
Examples of stressors include:
Infection.
Surgery.
Acute (sudden and severe) inflammation.
Ischemia (lack of blood flow to an area of your body).
Cancer
Key points:
SIRS is not a disease, it is a syndrome, a pattern of abnormal physiology.
It is highly sensitive, meaning it catches deterioration early.
It can be caused by infection (leading to sepsis) or non‑infectious triggers like trauma or pancreatitis.
Why SIRS Happens
SIRS is driven by a cytokine storm, a dysregulated release of inflammatory mediators.
Step-by-step pathophysiology:

It visually walks through the full inflammatory cascade: from Trigger → Cytokine Storm → Endothelial Injury → Capillary Leak → Microvascular Thrombosis → Organ Dysfunction, with clean clinical icons and a modern layout.
SIRS Criteria Infographic
A clean medical infographic showing the four SIRS criteria with icons: thermometer, heart, lungs, and WBC.
Trigger (infection, trauma, burns, ischemia, pancreatitis)
Immune activation
· Macrophages release TNF‑α, IL‑1, IL‑6
· Complement activation
Endothelial injury
· Capillary leakage
· Tissue edema
Microvascular thrombosis
· Platelet activation
· Coagulation cascade
Impaired oxygen delivery
· Mitochondrial dysfunction
· Organ hypoperfusion
Organ dysfunction
AKI
ARDS
Shock
This explains why SIRS can progress to sepsis, septic shock, or MODS
What’s the difference between SIRS and sepsis?
When the source of SIRS is an infection, it’s called sepsis. Sepsis is a life-threatening medical emergency caused by your body’s overwhelming response to an infection.
In other words, almost all people with sepsis have SIRS, but not all people with SIRS have sepsis.
How common is SIRS?
It’s difficult for researchers to estimate how common SIRS is because not all people with SIRS get to a healthcare facility in time. But SIRS is relatively common in emergency room departments and intensive care units (ICUs).
In one study that monitored almost 27,000 hospitalized people, 15% of them met at least two diagnostic criteria for SIRS when they first got to the hospital. About 47% of them met the criteria at least once during their hospital stay.
What are the symptoms of SIRS?
Several conditions can cause SIRS, and it can affect many different areas of your body. Because of this, SIRS has a wide variety of symptoms. They may include:
Redness and swelling (edema) in the affected parts of your body.
Intense pain.
Loss of function of parts of your body.
Intense fatigue.
Fast heart rate (tachycardia).
Abnormal breathing.
Shaking or chills.
Warm or clammy/sweaty skin.
Confusion, agitation or other mental changes.
Loss of consciousness.
If you have these symptoms, call 911 or get to the nearest emergency room as soon as possible. SIRS is a medical emergency.
What causes SIRS?
SIRS happens when your body’s immune system has an exaggerated response to a stressor. While your body normally uses inflammation to help you, this response is extreme, and the inflammation causes serious harm.
Several conditions and situations can trigger SIRS, some of which include:
Acute (sudden and severe) aspiration (when food, liquid or other material enters your airway and lungs).
Acute end-organ ischemia (lack of blood flow to an organ).
Acute pancreatitis.
An adverse reaction to a medication.
Blood cancers (hematologic malignancy), like leukemia, lymphoma and multiple myeloma.
Lack of blood flow to your intestines and gastrointestinal perforation.
Nonmedical substance uses and overdose.
Sudden worsening of vasculitis.
Trauma and surgery-related trauma.
Viral flu-like conditions.
Wide-spread fungal infections in people who have weak immune systems (immunosuppressed).
What are the risk factors for SIRS?
Risk factors for SIRS include:
Age: Infants and people over 65 are most at risk.
Weakened immune system: People with weakened immune systems, such as from cancer treatment, HIV or an organ transplant, are at increased risk.
Chronic conditions: Certain chronic conditions can put you more at risk, like diabetes, cirrhosis and COPD.
Existing infection: Having a current infection like pneumonia, meningitis or cellulitis increases your risk of SIRS.
SIRS Diagnostic Criteria

How SIRS is diagnosed
As SIRS is life-threatening, healthcare providers rely on the following to make a quick diagnosis:
Physical exam, including checking vital signs.
Your symptoms.
Your medical history.
The possible cause of SIRS (if known).
These strategies are usually enough for providers to suspect SIRS and start treatment right away. They’ll also order several tests to check your health and try to determine the cause of SIRS if they don’t already know it. These tests may include:
Blood tests, like basic metabolic panel, complete blood count (CBC), lactic acid test, liver function tests and kidney function tests.
Blood oxygen level.
Urinalysis.
Bacteria culture test.
Imaging tests, such as X-rays or CT scans.
SIRS criteria

To be diagnosed with SIRS, you must have two or more of the following:
Body temperature over 100.4 degrees Fahrenheit (38 degrees Celsius) or under 96.8 degrees F (36 degrees C).
Heart rate greater than 90 beats per minute.
Respiratory rate greater than 20 breaths per minute or partial pressure of CO2 less than 32 mmHg.
Leukocyte (white blood cell) count greater than 12,000.
The diagnostic criteria are different for children. They must have an abnormal leukocyte count or temperature to receive the diagnosis. This is because abnormal heart rate and respiratory rates are more common in children.
How is SIRS treated?
The management of SIRS involves treating the main cause and treatment that aims to prevent organ failure (multi-organ dysfunction syndrome, or MODS).
The treatment largely depends on the underlying cause but may include:
IV fluids to maintain blood flow to your organs and prevent your blood pressure from dropping too low.
Antibiotics (if you have a bacterial infection).
Vasopressor medications to reach healthy blood pressure.
Corticosteroids to prevent or reverse shock.
IV insulin to manage blood sugar levels (if necessary).
Surgery, such as for draining a wound infection, removing damaged tissue or exploratory surgery.
If organ failures occur, you’ll need other treatments such as dialysis for kidney failure or mechanical ventilation for respiratory failure.
What is the prognosis for SIRS?
The prognosis (outlook) for SIRS varies based on:
How quickly you receive a diagnosis and treatment.
The underlying cause of SIRS.
If you have risk factors for SIRS, like a weakened immune system.
With prompt treatment, many people with SIRS recover completely and return to leading normal lives. Up to 7% of people with SIRS die from the syndrome. The mortality rates for sepsis specifically are:
1.3% for sepsis.
9.2% for severe sepsis.
28% for septic shock.
Due to the risk of death, it’s important to get medical care as soon as you experience symptoms of SIRS.
What are the complications of SIRS?
SIRS can result in severe sepsis or septic shock (if the trigger is an infection) and multi-organ or single-organ failure. Other possible complications include:
Acute adrenal insufficiency (when your adrenal glands don't make enough of certain hormones, like cortisol).
Acute encephalopathy (any brain disease that alters your brain’s function or structure).
Acute respiratory distress syndrome (ARDS).
Acute transaminitis (high levels of certain enzymes that affect your liver function).
Acute tubular necrosis.
Deep vein thrombosis (DVT).
Disseminated intravascular coagulation (DIC).
Hemolysis.
Metabolic acidosis.
Thrombocytosis or thrombocytopenia.
Some of these complications may be treatable or reversible and some are permanent (like brain damage).
Can I prevent SIRS?
Steps you can take to try to prevent SIRS, include:
Regularly practicing good hygiene, including handwashing, to try to prevent viral infections.
Keeping cuts and other wounds clean while they heal.
Keeping up to date on recommended vaccines.
Getting routine medical care for chronic conditions.
Seeing your healthcare provider if symptoms of existing conditions or illnesses get worse.
Getting medical attention immediately if you have a serious injury or suspect an infection.
Clinical Presentation
Patients may show:
Fever or hypothermia
Tachycardia
Tachypnea
Confusion or agitation
Warm or cool skin
Hypotension
Elevated lactate
Abnormal WBC count
SIRS is often the first sign of sepsis or shock.
Complications of SIRS

If untreated, SIRS can lead to:
Sepsis (if infection present)
Septic shock
Acute kidney injury
ARDS
DIC
Multiple organ dysfunction syndrome (MODS)
Mortality increases dramatically once shock develops.

Management Principles
1. Treat the underlying cause
Antibiotics for infection
Surgery for perforation or abscess
Fluids for dehydration
Reversal of drug toxicity
2. Stabilize physiology
IV fluids
Vasopressors
Oxygen or ventilation
Blood sugar control
3. Monitor for organ dysfunction
Urine output
Lactate
Creatinine
LFTs
Mental status
SIRS vs Sepsis vs Septic Shock
SIRS Criteria Infographic
A clean medical infographic showing the four SIRS criteria with icons: thermometer, heart, lungs, and WBC.
BUTTERFLY CHART FOR SIRS IN TABLEAU — COMPLETE GUIDE
A butterfly chart is perfect for comparing SIRS vs No SIRS across age groups, units, or time.
1. Data Requirements
Patient ID
Age or Age Group
SIRS Count
SIRS Classification (SIRS / No SIRS)
Timestamp (optional)
2. Calculated Fields
Temperature Flag
IF [Temp] > 38 OR [Temp] < 36 THEN 1 ELSE 0 END
Heart Rate Flag
IF [HR] > 90 THEN 1 ELSE 0 END
Respiratory Flag
IF [RR] > 20 OR [PaCO2] < 32 THEN 1 ELSE 0 END
WBC Flag
IF [WBC] > 12000 OR [WBC] < 4000 OR [Bands] > 10 THEN 1 ELSE 0 END
Total SIRS Count
[Temp Flag] + [HR Flag] + [Resp Flag] + [WBC Flag]
SIRS Classification
IF [Total SIRS Count] >= 2 THEN "SIRS" ELSE "No SIRS" END
3. Building the Butterfly Chart
Step 1 Create Age Groups
IF [Age] < 20 THEN "0–19" ELSEIF [Age] < 40 THEN "20–39" ELSEIF [Age] < 60 THEN "40–59" ELSEIF [Age] < 80 THEN "60–79" ELSE "80+" END
Step 2 Create Two Measures
IF [SIRS Classification] = "SIRS" THEN 1 END
IF [SIRS Classification] = "No SIRS" THEN 1 END
Step 3 Make One Side Negative
-[SIRS Count]
Step 4 — Build the Chart
Rows → Age Group
Columns → SIRS Count (negative) and No SIRS Count (positive)
Color → SIRS Classification
Label → Count
Sort → Age Group ascending
Step 5 Add Center Axis
Dual axis
Synchronize
Hide headers
4. Interpretation
A butterfly chart helps clinicians instantly see:
Which age groups have the highest SIRS burden
Whether SIRS is clustering in older or younger patients
Whether interventions are reducing SIRS over time
5. Image‑Ready Description for Butterfly Chart
A mirrored bar chart with age groups in the center, SIRS counts on the left (red bars), and No SIRS counts on the right (green bars).
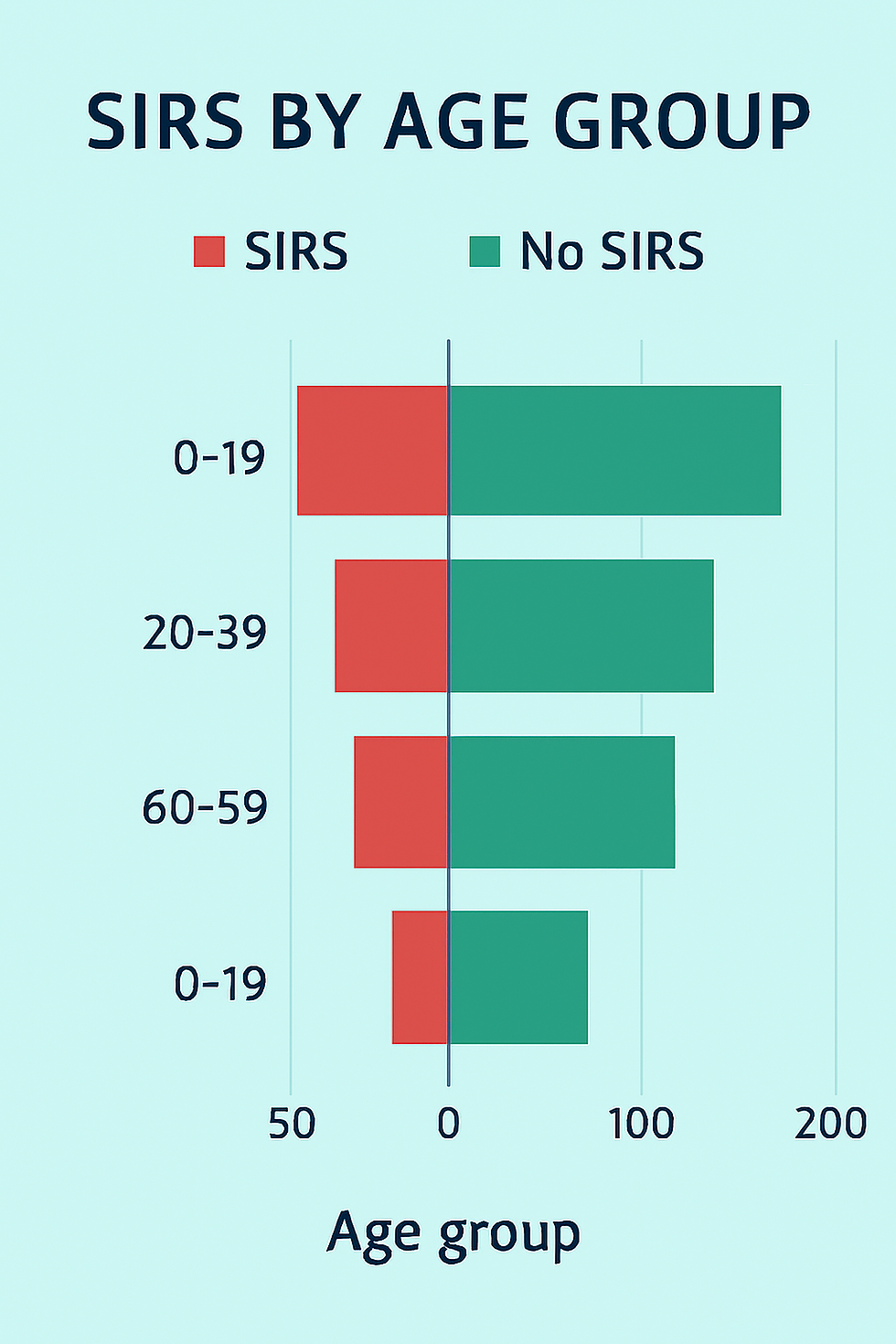
Butterfly Chart Explanation: SIRS vs No SIRS by Age Group
Center axis: Age groups (0–19, 20–39, 40–59, 60–79, 80+)
Left side (Red bars): Number of patients who met SIRS criteria (≥2 abnormal findings)
Right side (Green bars): Number of patients who did not meet SIRS criteria
This mirrored layout creates a “butterfly” effect, making it easy to compare both groups side by side.

Clinical Insights
60–79 age group shows the highest number of SIRS cases, indicating increased inflammatory risk in older adults.
Younger groups (0–39) have fewer SIRS cases, suggesting better physiological resilience.
80+ group shows high SIRS counts but lower total volume, possibly due to smaller cohort size or early mortality.
Key Takeaways
SIRS is a medical emergency because unchecked inflammation can rapidly progress to organ dysfunction, sepsis, or shock.
It is defined by meeting two or more physiologic criteria: abnormal temperature, heart rate, respiratory rate, or white blood cell count.
SIRS can be triggered by infection, trauma, burns, pancreatitis, ischemia, or other major stressors.
When SIRS is caused by infection, it becomes sepsis, but SIRS can occur without infection as well.
Early recognition and treatment—fluids, source control, antibiotics (if infection), and organ support—are essential to prevent deterioration.
Conclusion
SIRS is best understood as the body’s red‑alert mode—a sign that the immune system is in overdrive. Recognizing it early can save lives, guide timely interventions, and prevent progression to severe sepsis, septic shock, or multi‑organ failure.